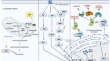
Overview
EPMA Journal publishes results and achievements in primary (individualised protection of healthy persons against health-to-disease transition) and secondary (individualised protection against disease progression) care
- Focused on paradigm change from reactive medicine to cost-effective predictive approach, targeted prevention and treatments tailored to the person.
- This type of research and medical care is complex and requires multi-professional expertise.
- Application of patient-friendly non-invasive diagnostics and innovative treatment algorithms tailored to the individualised patient profile is envisaged.
- Innovative technology development follows the concept “From Bench to Bedside”.
- Official journal of the European Association for Predictive, Preventive and Personalized Medicine, EPMA, Brussels.
- Editor-in-Chief
-
- Olga Golubnitschaja
- Impact factor
- 6.5 (2022)
- 5 year impact factor
- 5.3 (2022)
- Submission to first decision (median)
- 7 days
- Downloads
- 427,841 (2023)
Societies and partnerships

Latest issue
March 2024 |Predictive, Preventive and Personalised Approach in Primary and Secondary Healthcare; Special issue – Internationally awarded research innovation
Latest articles
Journal updates
-
Editor-in-Chief Highlights: September 2023
View the latest Editor-in-Chief highlights from EPMA Journal.
-
Editor-in-Chief Highlights: June 2023
View the latest Editor-in-Chief highlights from EPMA Journal.
-
Editor-in-Chief Highlights: June 2022
View the latest Editor-in-Chief highlights from EPMA Journal.
-
Editor-in-Chief Highlights: March 2022
View the latest Editor-in-Chief highlights from EPMA Journal.
Journal information
- Electronic ISSN
- 1878-5085
- Abstracted and indexed in
-
- ANVUR
- Baidu
- CAB Abstracts
- CLOCKSS
- CNKI
- CNPIEC
- Current Contents/Life Sciences
- Dimensions
- EBSCO
- EMBASE
- Gale
- Google Scholar
- Japanese Science and Technology Agency (JST)
- Meta
- Naver
- Norwegian Register for Scientific Journals and Series
- OCLC WorldCat Discovery Service
- Portico
- ProQuest
- Psyndex
- PubMedCentral
- Reaxys
- SCImago
- SCOPUS
- Science Citation Index Expanded (SCIE)
- TD Net Discovery Service
- UGC-CARE List (India)
- Wanfang
- Copyright information
-
© European Association for Predictive, Preventive and Personalised Medicine (EPMA)